Amanda Burrill has practically lived several lifetimes in one. She has worked as a rescue swimmer in the Navy, as a model and actress, as a Cordon Bleu-trained chef, as a sports copy editor for the New York Post, as an on-air host for the Travel Channel, and as a sponsored triathlete and marathon runner. She is a mountaineer, now more than halfway toward her goal of climbing all the Seven Summits by spring 2023.
“I get all this credit for being this adventurous Renaissance woman,” Burrill, 42, said. “But I know the real story.” Through most of her endeavors, “there was a lack of intent,” she said. “It was surviving. But it was surviving in style.”
For many years, she skipped from one occupation to another to hide the symptoms of a traumatic brain injury. Just as she was about to lose her footing with one, she would gracefully pivot to another rather than stumble.

She didn’t know she had a brain injury. She only knew that important cognitive functions were slipping away from her. She started finding it hard to read and process information. Her hand-eye coordination was off. Her feelings toward her husband suddenly changed.
“It would be bad enough to say, ‘I don’t love my husband anymore,’” said Burrill. “But to feel that and not understand why—but have a very clear reason why—I felt horrible, and a lot of shame.” When she returned home from a deployment in July 2003, she divorced him, although she says that he was the one person who would have been “able to observe me and say something serious has changed.”
She didn’t connect her symptoms with her fall down the hatch of a prison ship in 2003. It was during her tour to Iraq, and no one was around to witness the fall; she was found lying unconscious on the deck afterward. Her doctors didn’t make the connection, either. The Veterans Affairs (VA) system eventually chalked up her symptoms to various conditions, including post-traumatic stress disorder (PTSD) and fibromyalgia.
“Post-traumatic stress disorder was a convenient catch-all diagnosis to explain away all my symptoms,” Burrill said. Yet she didn’t feel deeply traumatized by her wartime experiences. And the medications they gave her didn’t improve her condition. So many of her symptoms couldn’t be explained by PTSD alone. “A lot of things were off here and there, mystery issues, and I couldn’t connect the dots,” she said.
Thirteen years passed before she discovered that traumatic brain injury was the root cause behind her ailments. Throughout those years, she hid her symptoms out of shame while she fought through the medical system to find doctors who would look for the physical cause and stop telling her she just had psychiatric problems.
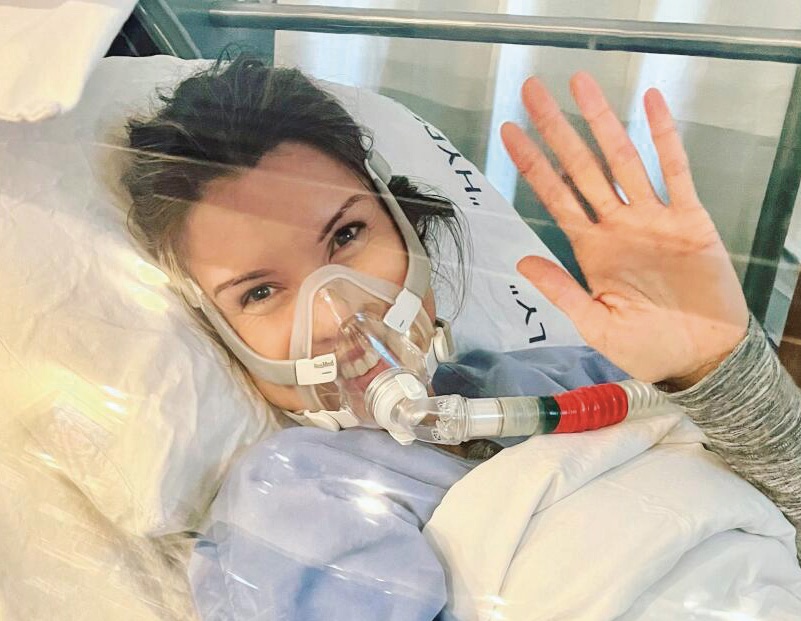
“A big part of my brain injury story was people not listening to or believing me,” said Burrill, who feels more traumatized by her experiences in doctors’ offices than from the war.
Since 2016, when she was finally diagnosed, she has striven forward with healing, seeking cutting-edge treatments and putting great effort into her rehabilitation. During her outstanding recovery, “they were calling me ‘star pupil,’ an ‘amazing case,’” Burrill said. She has come far, but said “that doesn’t mean I feel all better.” As she continues her healing journey, she has become an advocate for veterans and others with traumatic brain injury.
In Hiding, Even From Herself
Between her brain injury in 2003 and the end of her military service in 2007, she didn’t talk about her symptoms much, even to doctors.
“I’d report things like bike crashes and digestion issues, but not the emotional duress. This was before you could have mental issues and stay in the military,” Burrill explained. “People were getting discharged—other than honorable—for having mental health issues.” It’s gotten better now, she says, but at the time, “I had to stay really mum about the emotional duress.
“I think I was even denying myself the ability to really process, like, ‘Hey, I’m struggling here.’ That wasn’t really allowed because of the way I was raised and then the military culture,” Burrill said. Her father, who was in the Navy, trained her to be strong and to be a star athlete. He guided her away from piano lessons and other pursuits of a softer nature. To admit she was ailing felt like weakness.
When Burrill found that she could no longer effectively complete nightly briefings as an intelligence officer, she tried to hide it by changing roles. Banking on what was left of her athleticism, she asked if she could undergo the notoriously grueling training for Navy rescue swimmers. Her command eventually agreed to it, and she passed.
Burrill had planned to go to law school when she finished her military service. She knew that was no longer possible due to the mysterious change that had come over her. Burrill identified her next career move using what she calls “the Venn diagram of my adult life: What am I good at and what am I interested in, and where do those things overlap?” Cooking was her first answer. Her mother, a Vietnamese refugee, was a caterer, and Burrill primarily learned about cooking from her.
Burrill studied at the eminent Le Cordon Bleu culinary arts institute in Los Angeles. Her success was again shadowed by mysterious shortcomings. “Why am I so bad at cutting things?” she asked herself. Her coordination and vision were affected by her brain injury. She nonetheless made it through and landed a coveted position in the test kitchen at the Los Angeles Times. That guided her next pivot, toward journalism.

Burrill felt it was only a matter of time before she could no longer overcome her limitations. So, she went to the Columbia University Graduate School of Journalism and received a master’s degree. Focusing on sports and travel journalism allowed her to avoid research as much as possible and write from her own knowledge.
She was the first woman to get a job in editorial for the New York Post sports section. But she struggled with various aspects of the job, and it was even hard for her to figure out how to fill out her timesheets to get paid. “I always felt like I was at risk of being found out,” Burrill said.
Running has been a comfort and also a source of income along the way. She has completed over 25 marathons and triathlons, including two Ironman races. Prioritizing sports and fitness also landed her in the world of fitness modeling, and she appeared twice on the cover of Runner’s World magazine.
The mysterious illness that dimmed all her shining accomplishments hung thick over her athleticism, as well. “I had tried to continue being a marathoner and triathlete through all of this and it really came at great detriment to my body,” Burrill said. Her brain injury had caused issues with blood flow, nerve damage, and muscle wasting. She also believes the assortment of medications she was taking, most for conditions she didn’t have, may have affected the structural integrity of her body.
Burrill sustained many injuries, the worst of which was the collapse of her foot’s arch during the Chicago Marathon in 2015. “I was basically in a boot or cast or on crutches for 17 months,” she said. She had surgery that put a metal plate in her foot, which ended her running career.
In February this year, she had knee surgery—the most recent of some 20 surgeries she has had. Before her brain injury, she had always been fit and had little to no experience with medical care.

A Second Brain Injury
Several months before her Chicago Marathon injury, Burrill fell on the stairs in her apartment building in New York and hit her head on a marble wall. She visited a nurse practitioner at her local VA clinic. “He was just like, you know, ‘You got your bell rung,’” she said. It wasn’t treated as a big deal.
“My problems got progressively worse. It was like my old problems, but like these problems I had all along on steroids,” Burrill said. During a visit to the VA hospital, she discovered that each clinic has a social worker to help veterans with questions and various issues. “You don’t know these things when you can hardly read or look at a screen,” she added.
She walked right into the social worker’s office. He was the first person to suggest screening her for traumatic brain injury (TBI). The scope of TBI among veterans has become better understood over the years; the Defense and Veterans Brain Injury Center reported more than 400,000 TBIs among U.S. service members from 2000 to late 2019.

The screening led to further tests and, finally, in 2016, a diagnosis. Doctors pegged her 2003 fall—along with her more recent fall and potentially some tumbles on her bike—as having caused injury to her brain.
During the testing, she was found to be exceptionally high-functioning in many areas, but she was in the bottom 5 percent for six areas, including visual orientation and working memory.
Finding and addressing the root cause has helped remedy Burrill’s symptoms, which have included poor digestion, poor kidney function, and problems with her endocrine system. The brain affects so much in the body, and TBI affects each person differently, which has made diagnosis difficult, and many vets have been similarly misdiagnosed.
Reaching New Heights
Burrill describes some of the treatments that have helped her regain much of what she lost. “It sounds almost like kindergarten games. At CognitiveFX, in Utah, I would do things like stomp and keep a beat while I had a woman standing next to me, and she would pull out a card—let’s say it’s the letter R on the card—and I would have to say 10 words that start with the letter R.
“Basically, you’re multitasking in a way that drives blood to this area of the brain that isn’t getting enough blood. It’s not necessarily that the brain is broken there still; it may be healed, but it’s just that the blood has a comfortable path that it’s used to.”
The left occipital lobe, a part of her brain that was injured, affects vision. She got special glasses from The Mind-Eye Institute, near Chicago, that bend the light so it hits her retina in a different way and brings the information to a different part of her brain that isn’t damaged.

In retrospect, Burrill said, her jumping from occupation to occupation also helped even before she knew she had a brain injury. “Brains love novelty,” she observes—working as a travel writer, for example. “Think about it. When you go to a new place, even just figuring out the way a new metro system works—that’s a brain workout.”
When Burrill was recovering from her major foot injury, “I was thinking about this metaphor, ‘If you can’t run, walk; if you can’t walk, crawl,’” she says. She couldn’t be a runner anymore, so she thought, “Why not walk?” She set her sights on hiking, though she had never been much of a hiker.
“I don’t like to do things small,” Burrill said. She thought, “How cool would it be if my first hike ever was to go to Tanzania and hike Kilimanjaro?” Africa’s highest peak, Mount Kilimanjaro is one of the world’s Seven Summits.
“I had a profound experience over the seven days I was climbing Kilimanjaro. I had no devices, no distractions. My job was to put one foot in front of the other, tolerate the cold, and just be present.”
She went on to Denali, another of the Seven Summits. Successfully self-guiding that mountain made her realize, “I’m not just good at this for a disabled person or ‘adaptive athlete,’ as I was being called; I’m good at this, period.”
She is set to finish all Seven Summits by spring 2023. Mount Everest, the highest, will be last. Even sitting with ice on her knee, still recovering from surgery, Burrill spoke confidently of the great climbs ahead.
“For a while, I was using mountaineering as outward proof that I was getting better,” she said. “I don’t need to do that anymore. I do this because I love it. I love going to a new place and doing something hard, and in the meantime, I have peace. It’s nature therapy.”
This article was originally published in American Essence magazine.













